US faces major hurdles for COVID-19 vaccine distribution: Vaccine advisory committee
Any coronavirus vaccine that could be authorized for emergency use by the U.S. Food and Drug Administration (FDA) faces several additional hurdles after completing the final stage of clinical trials.
That was the theme of key issues addressed today by the FDA’s vaccine advisory committee — which includes a group of health and science experts who advise the regulatory agency on the best way to approach the path forward for a COVID-19 vaccine.
Among the more immediate hurdles, the path to receive an emergency use authorization remains somewhat murky for the pharmaceutical industry, as the agency has not nailed down specifics for things such as labeling and what qualifies as sufficient monitoring of individuals who have enrolled in clinical trials.
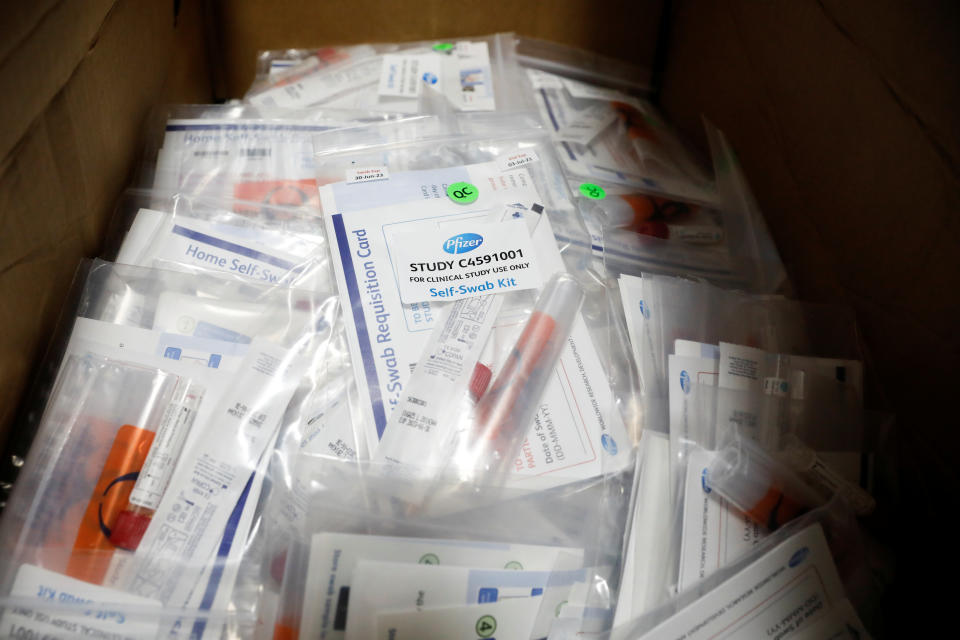
In separate letters to the committee, Pfizer (PFE), Johnson & Johnson’s (JNJ) Janssen and trade group BIO all asked for more clarity on the follow-up period for participants following the final dose of the vaccine.
J&J wrote that the current guidelines ask for 50% of the trial population to be monitored for two months following the final dosing. With J&J enrolling 60,000 participants, and other competitors only enrolling 30,000, that provides an uneven playing field.
“Specifying a minimum required follow-up in terms of subjects and months ... would ensure consistency across all studies,” the company wrote.
Another concern is what happens to trial participants — especially in a placebo group — after an emergency use authorization is awarded. The FDA’s guidelines require that the placebo group is maintained so that collection of data for safety and efficacy continues on through until the vaccine can be fully approved — especially since the vaccine would still be considered “investigational” at the point.
Pfizer had said it anticipates offering the vaccine to the placebo participants once it receives an emergency use authorization (EUA) — which is an ethical obligation, according to BIO.
“Additional discussion is needed to determine how placebo-controlled trials can be maintained after an EUA is granted. As an industry, we have an ethical obligation to make our trial participants aware that a vaccine may be available,” wrote BIO’s senior director of infectious disease policy Gregory Frank.
FDA’s deputy director of vaccines, Doran Fink, said the trial has to remain blinded because that isn’t a step that can be walked back and it could jeopardize the integrity of the massive trials.
When asked what can be done to ensure that participants don’t simply then drop out of the trial or choose to take the vaccine, Fink said the FDA had no idea and is asking the companies to figure it out and describe their plan in any emergency use authorization filings.
Distribution and administration
What happens after an EUA is also of concern, as the distribution process for two frontrunners — Moderna (MRNA) and Pfizer — requires extra cold temperatures. While Moderna has emphasized it has been able to make its “extra” cold the temperature of a normal house freezer, the distribution process remains uncertain.
The CDC’s medical officer in the division of viral diseases, Janell Routh, said hospitals and clinics do not need to purchase their own cold storage equipment because if a vaccine is authorized, the manufacturers will be responsible for maintaining the vaccine in storage. As part of the authorization, the companies will also have to prove that the vaccine can be safely transported and kept until the expiry date without losing integrity in the product.
Administration
Yet another obstacle is the public’s low confidence in the process, as well as proper administration of two-dose vaccines. The frontrunners both require two doses, which means a second shot after 28 days is required in order for the vaccine to be effective.
To that end, the CDC intends to launch a platform that will text reminders to recipients, as well as provide a vaccine card that can help medical professionals ensure they receive the booster shot from the same company as the first dose — since there has been no trial to test if the vaccines from two different companies combined provide the same level of protection.
However, there is no way to mandate or ensure that both doses are administered. The only vaccine among those in the lead that requires only one dose is from Johnson & Johnson.
To help ensure residents of long term care facilities are able to receive a vaccine, as they are in the first level of priority, the government has already partnered with pharmacies CVS (CVS) and Walgreens (WBA) to offer clinical experts on site, on a voluntary basis, to administer the vaccine. CVS is hiring this quarter with a similar role envisioned at their sites for the general public — but that hasn’t been announced by the government yet.
Routh noted that pharmacies could play a key role in administration, since 90% of Americans live within 10 miles of a pharmacy.
Vaccine confidence
Another issue that health agencies are scrambling to address is confidence in any vaccine. Hurdles include a general mistrust of the federal government’s handling of the process and historical fears in certain communities, according to the Reagan-Udall Foundation — which presented sobering findings from listening sessions with frontline workers and underserved populations, such as minorities.
The foundation, a non-profit arm of the FDA, found a strong mistrust among under-served communities, of players’ incentives — political and economical— as well as historical concerns.
“Doctors are going to be pushed to sell this (vaccine) to our community. I would like you to not sell me, but show me and tell me, educate me,” was one of the comments the Foundation heard.
Other participants said they felt like guinea pigs for the wealthy.
The Foundation plans to craft messaging by December that the FDA can use to penetrate these communities and help encourage more people to take the vaccine.
With the first filings for an EUA anticipated in November, the agencies are nearing the deadline to iron out the details to inoculate as many of the more than 330 million Americans as possible.
More from Anjalee:
Redfield: CDC 'preparing earnestly' for vaccine in November, December
India's tech giants navigate 'literally spiking' WFH demand, H1-B fears in coronavirus era
How protests spurred Corporate America into action on race, inequality
Read the latest financial and business news from Yahoo Finance
Follow Yahoo Finance on Twitter, Facebook, Instagram, Flipboard, SmartNews, LinkedIn, YouTube.

 Yahoo Finance
Yahoo Finance 